Disaster Preparedness, Response, at Recovery sa Community Health Nursing
Mahahalagang Punto
- Pinagsasama ng disaster management ang preparedness, mitigation, response, at recovery sa tuloy-tuloy na cycle.
- Dapat kasama sa RN disaster planning ang social vulnerability analysis dahil hindi pantay ang catastrophic impact sa mga populasyon.
- Binibigyang-priyoridad ng response operations ang lifesaving care, access sa shelter/food/water, at maagang psychological stabilization.
- Inilalaan ng field triage at disaster triage (halimbawa START) ang limitadong resources sa panahon ng surge events.
- Nangangailangan ang chemical at environmental exposure events ng mabilis na contamination-risk assessment at decontamination decisions upang maiwasan ang secondary harm.
- Higit pa sa infrastructure repair ang recovery at nangangailangan ng monitoring para sa PTSD, pagtaas ng substance use, at suicide risk.
- Nakasalalay ang disaster readiness sa handang nursing workforce na kinabibilangan ng active, reserve, retired, at volunteer nurses sa civilian at uniformed systems.
- Kabilang sa environmental disasters ang weather- at geologic-hazard pathways (halimbawa floods, hurricanes, tsunamis, earthquakes, landslides, at wildfires) na maaaring mabilis na humarang sa access sa care.
- Kabilang sa biological disasters ang infectious outbreaks, pandemics, at deliberate biologic release events na nangangailangan ng mabilis na surveillance at infection-control escalation.
- Kabilang sa technological disasters ang chemical, radiological, nuclear, at cyber/infrastructure failures na maaaring mabilis na makagambala sa patient safety at care delivery systems.
- Nangangailangan ang bioterror readiness ng maagang pagkilala sa unusual exposure signals at mabilis na reporting sa local health-department at CDC/public-health channels.
- Nangangailangan ang epidemic at pandemic response ng maagang pattern recognition (point-source, propagated, mixed transmission), mabilis na triage/isolation, at tuloy-tuloy na community risk communication.
- Malakas ang impluwensiya sa bisa ng outbreak communication ng perceived risk factors at trustworthiness ng communicator.
- Ipinapakita ng historical pandemic patterns na malaki ang epekto sa mortality trajectories ng maaga at consistent na nonpharmacologic interventions at sapat na nursing workforce capacity.
- Bumababa ang kalidad ng pandemic response kapag ang stigma ay nagdudulot ng delayed care, hindi pantay na treatment access, o mistrust sa affected communities.
- Nakasalalay ang community disaster resilience sa coordinated phase-based action (mitigation, preparedness, response, recovery) at culturally inclusive planning.
- Nakasalalay ang hospital preparedness sa paulit-ulit na disaster training, performance evaluation, at role clarity sa loob ng incident command structure.
- Iniaayon ng mass-casualty triage tags ang urgency sa resource limits at nangangailangan ng mabilis na reassessment habang nagbabago ang kondisyon ng pasyente at capacity.
- Nakasalalay ang hospital readiness sa panahon ng disasters sa surge-capacity expansion, infection-control containment, at maaasahang internal/external emergency communication.
- Lumilikha ang mass-violence incidents (halimbawa active-shooter at terrorism events) ng malawak na psychosocial injury at fear burden na lampas sa direct casualties.
Pisyopatolohiya
Lumilikha ang disasters ng pinagsamang physical, environmental, at psychological injury load sa antas ng populasyon. Naitutulak ang health impact ng exposure intensity, baseline community vulnerability, at local response capacity.
Lumalala ang nursing outcomes kapag mahina ang preparedness at coordination. Ang maagang pag-organisa ng communication pathways, triage, hazard control, at behavioral health support ay nagpapababa ng avoidable morbidity at mortality.
Klasipikasyon
- Preparedness: Pre-event planning, risk mapping, training, at education para sa malamang na hazards.
- Mitigation: Mga aksyon na nagpapababa ng hazard probability at downstream severity bago ang impact.
- Response: Agarang post-event lifesaving operations, stabilization, at essential-needs support.
- Recovery: Pangmatagalang pagpapanumbalik ng services, infrastructure, at psychosocial function.
- Community-response-phase domain: Phase-based cycle ng mitigation, preparedness, response, at recovery na ginagamit para isaayos ang local disaster action.
- Social-vulnerability domain: Community characteristics (halimbawa poverty, transport barriers, crowding, age/disability concentration) na nagpapataas ng disaster risk at nagpapabagal ng recovery.
- Triage domain: Field triage/disaster triage processes na ginagamit upang bigyang-priyoridad ang limitadong treatment at transport capacity.
- Triage-tag domain: Color-coded class assignment (red immediate, yellow urgent, green delayed/ambulatory, black expectant) na ginagamit para idirekta ang scarce resources sa ilalim ng mass-casualty standards.
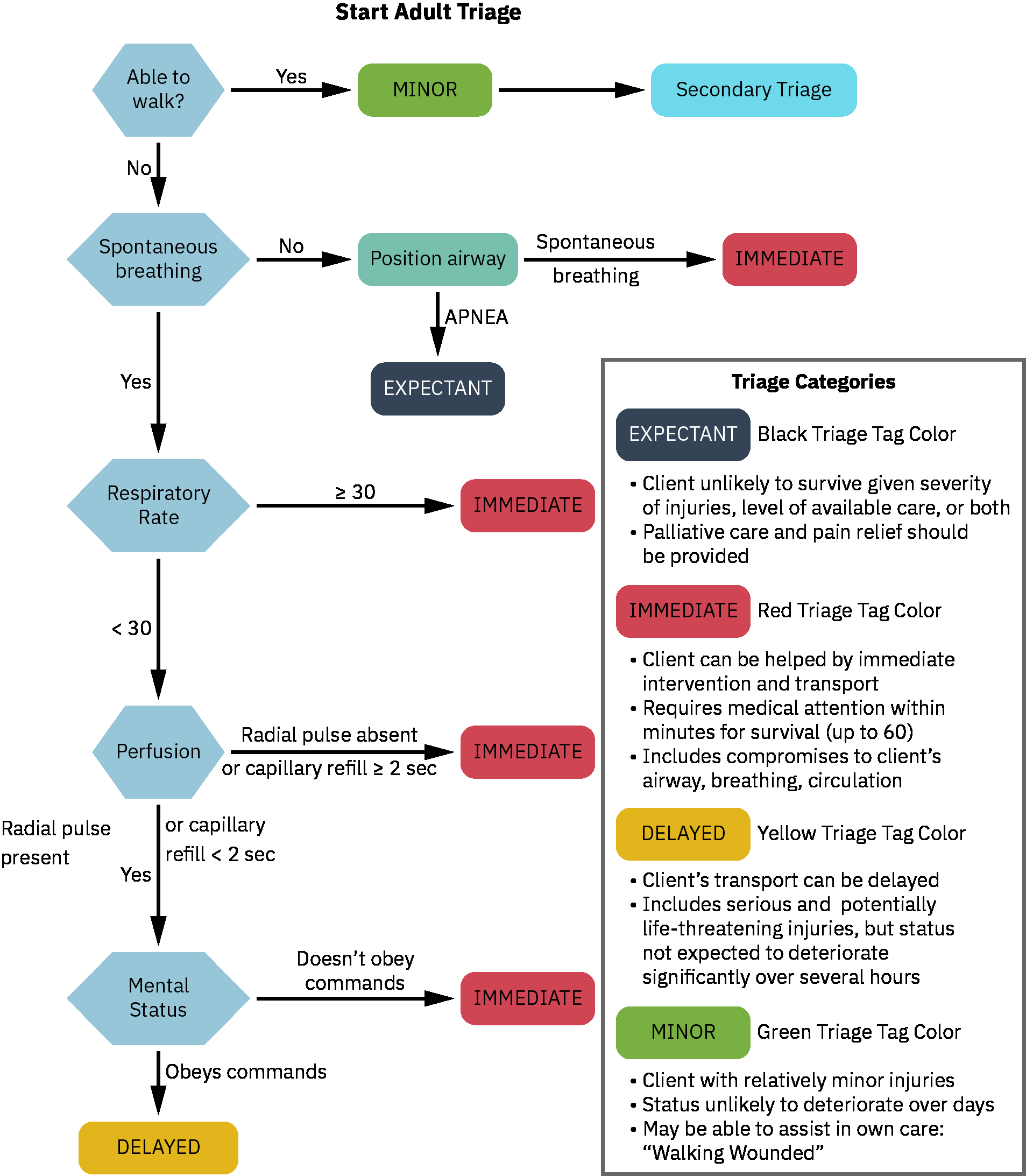 Illustration reference: OpenStax Population Health for Nurses Ch.32.5.
Illustration reference: OpenStax Population Health for Nurses Ch.32.5.
- Hazard-exposure domain: Chemical, biologic, at environmental exposures na nangangailangan ng contamination control at targeted treatment pathways.
- Environmental-hazard domain: Water-related disasters (storm surge, flash flooding, snowmelt flooding, tsunami) at land-related disasters (earthquake, landslide, wildfire) na lumilikha ng magkakaibang evacuation at infrastructure-failure patterns.
- Weather-alert domain: Ang
watchay nangangahulugang paborable ang kondisyon; angwarningay nangangahulugang nalalapit o kasalukuyang hazard na nangangailangan ng agarang protective action. - Biological-disaster domain: Infectious disease outbreaks, pandemics, at bioterrorism scenarios na nangangailangan ng syndromic surveillance, case reporting, at surge infection-control operations.
- Bioterror-mass-exposure domain: Ang maagang recognition, PPE-protected assessment, decontamination-zone setup, command communication, at mabilis na triage/transport ay nagpapababa ng secondary spread at mortality.
- Federal-countermeasure domain: Ang Strategic National Stockpile at medical countermeasures (vaccines, antimicrobials/antivirals/antidotes, diagnostics, at PPE) ay sumusuporta sa short-term surge gaps sa public-health emergencies.
- Outbreak-scale domain: Ang
epidemicay tumutukoy sa above-expected regional disease occurrence; angpandemicay tumutukoy sa international spread sa maraming countries/regions. - Outbreak-pattern domain: Point-source outbreaks (single shared exposure), propagated outbreaks (person-to-person spread), at mixed outbreaks (pinagsamang mechanisms).
- Risk-perception determinant domain: Nag-iiba ang uptake ng outbreak messages batay sa kung ang risks ay voluntary versus imposed, controllable versus externally controlled, familiar versus novel, at trusted-source versus untrusted-source.
- Risk-communication credibility domain: Ang empathy/caring, honesty/openness, dedication/commitment, at demonstrated competence ay nagpapataas ng public adherence.
- Historical-pandemic lesson domain: Paulit-ulit na ipinapakita ng mga nakaraang pandemics ang pagkalat sa mobility/crowding networks at delayed control kapag fragmented ang response implementation.
- Nonpharmacologic-control bundle domain: Isolation, quarantine, masking, distancing, hygiene/disinfection, at movement restrictions ang core controls kapag unavailable o delayed ang vaccines/therapeutics.
- Workforce-surge equity domain: Ang nursing shortages at inequitable workforce utilization ay nagpapababa ng response capacity at nagpapalala ng outcomes sa severe waves.
- Stigma-equity domain: Ang stigmatizing labels at exclusionary messaging ay nagpapababa ng testing, disclosure, treatment engagement, at equitable care access sa prolonged infectious crises.
- Prolonged-pandemic management domain: Ang ilang pandemics ay nagta-transition sa long-duration global burdens na nangangailangan ng sustained surveillance, treatment access, at prevention adaptation sa halip na short-wave response lamang.
- High-consequence-outbreak domain: Ang severe pathogens (halimbawa Ebola virus disease) ay nangangailangan ng mahigpit na exposure control, high-level PPE reliability, at protected handling sa high-risk body-fluid exposure contexts.
- Technological-disaster domain: Industrial/transport/infrastructure incidents, cyberattacks, at utility failures na maaaring mauwi sa chemical/radiological exposure at documentation-system downtime.
- Radiological-nuclear domain: Radiation exposure events na may acute at delayed morbidity, long-term contamination risk, at sustained public-health monitoring needs.
- Workforce-readiness domain: Staffing at competency capacity sa clinical settings, public-health systems, at volunteer response networks.
- Personal-preparedness domain: Individual nurse planning para sa family communication, transportation access, at role activation expectations sa panahon ng disasters.
- Culture-of-preparedness domain: Multilingual risk communication, culturally appropriate shelter operations, at community-leader engagement upang mapabuti ang trust at participation sa panahon ng krisis.
- Hospital-preparedness domain: Facility emergency planning na nagsasama ng staff training, competency evaluation, communication pathways, at resource allocation workflows.
- Incident-command domain: Structured command framework na tumutukoy ng roles, reporting, at decision authority sa emergency operations.
- NIMS/ICS domain: Gumagamit ang multiagency response ng common terminology at defined command roles (incident commander, operations, planning, logistics, finance/administration, liaison, safety, at intelligence/investigation functions).
- Zone-of-care domain: Sa CBRN-capable events, maaaring kailanganin ang paghihiwalay ng hot (direct contamination), warm (triage/decontamination), at cold (treatment/holding) zones.
- Drill-evaluation domain: Tabletop, simulation, at skills-based drills na sinusundan ng debrief at corrective-action planning upang mapabuti ang operational readiness.
- Surge-capacity domain: Expansion ng care areas, staffing, at supplies upang masalo ang patient volume na lampas sa normal operations.
- Emergency-communication domain: Policy-driven internal staff communication kasama ang external coordination sa families, responders, at community partners sa panahon ng krisis.
- Infection-control-surge domain: Outbreak/disaster containment gamit ang isolation precautions, PPE, environmental cleaning, at patient cohorting.
Pagsusuri sa Pag-aalaga
Pokus sa NCLEX
Unahin muna ang immediate life threats, pagkatapos suriin ang vulnerability, contamination risk, at behavioral health burden.
- Suriin ang disaster type at malamang na hazard profile (natural, man-made, infectious, o mixed exposure).
- Suriin ang social vulnerability factors na maaaring maglimita sa evacuation, resource access, at recovery capacity.
- Suriin ang local hazard profile at seasonality (halimbawa severe storms, heat burden, wildfire risk, earthquake/landslide exposure, at flood-prone terrain).
- Suriin ang kasalukuyang phase ng disaster management upang maitugma ang intervention priorities.
- Suriin ang early biologic-threat cues (clustered febrile illness, unusual severity patterns, rapid community spread, o atypical exposure history) at i-report ayon sa protocol.
- Sa posibleng bioterror contexts, suriin ang sentinel indicators tulad ng unusual dead/dying animals, unexplained severe illnesses/deaths, atypical vapors o odors, at unusual insect swarms.
- Suriin ang probable outbreak pattern at transmission dynamics (shared-source cluster versus sustained person-to-person spread) upang gabayan ang containment priorities.
- Suriin ang availability ng communication, coordination, at collaboration assets sa pagitan ng health agencies at community partners.
- Suriin kung isinasaalang-alang ng response plans ang language access, cultural practices, at trusted local leadership na kailangan para sa equitable emergency communication.
- Suriin ang perceived-risk drivers sa target audience (control, familiarity, expected benefit timing, at trusted messenger).
- Suriin ang nursing workforce readiness, kabilang ang surge staffing options, role clarity, at just-in-time competency needs para sa disaster deployment.
- Suriin kung may equitable at full workforce mobilization ang surge staffing plans upang maiwasan ang avoidable staffing gaps.
- Suriin ang hospital emergency-policy readiness, kabilang ang incident-command role assignment, internal/external communication flow, at resource-allocation triggers.
- Suriin ang recent drill at debrief findings upang matukoy ang unresolved competency gaps sa triage, communication, at team coordination.
- Suriin ang personal disaster-readiness conflicts para sa deployed nurses (duty-to-care versus family safety obligations) bago pa maganap ang events.
- Suriin ang triage category at clinical trajectory gamit ang established mass-casualty protocols kapag active ang surge standards.
- Sa mass-violence/MCI response, unahin ang pagsusuri sa scene-security status (halimbawa active offender, secondary explosive risk, at collapse/fire hazards) bago clinical approach.
- Suriin ang class-specific triage urgency at expected treatment window upang maprayoridad ang immediate versus delayed care needs.
- Suriin kung ang ambulatory green-tag patients ay maaaring makaalis sa screening areas habang may contamination risk pa rin sa ibang environments.
- Suriin ang contamination indicators: exposure symptoms, visible residue sa skin/clothing, proximity sa release site, at detection-device results.
- Suriin ang pangangailangan sa decontamination upang maprotektahan ang pasyente, staff, first receivers, at nakapaligid na care infrastructure mula sa secondary contamination.
- Suriin ang surge-capacity readiness, kabilang ang expandable treatment spaces, supplemental staffing plans, at high-volume resource-allocation triggers.
- Suriin ang disaster infection-control readiness (isolation flow, PPE supply, environmental cleaning throughput, at cohorting feasibility) sa panahon ng high census.
- Suriin ang emergency communication reliability para sa internal command updates at external messaging sa patients, families, EMS, at community agencies.
- Suriin kung ang stigma, discrimination, o misinformation ay nagpapababa ng help-seeking, testing uptake, o adherence sa affected populations.
- Suriin ang access-to-care disruption risk (blocked roads, damaged facilities, communication failure, electrical power loss, at interruption ng home medications/equipment).
- Suriin ang technological-dependency failures (EHR downtime, communication-system compromise, device/equipment malfunction) na maaaring magbago ng triage at medication safety workflows.
- Suriin ang survivor emotional status para sa fear, anxiety, despair, at functional decline sa response at recovery periods.
- Sa infectious-disease emergencies, suriin ang screening/testing throughput, vaccine-distribution workflow, at transmission-precaution reliability.
- Sa recovery period, suriin ang delayed behavioral sequelae kabilang ang PTSD symptoms, substance misuse, at suicide-risk cues.
Mga Interbensyon sa Pag-aalaga
- Bumuo ng preparedness plans na nagsasama ng hazard analysis, staff training, at community education.
- Gumamit ng recurring hospital preparedness drills (tabletop, functional, at full-scale multiagency exercises) na may post-drill debrief upang maisara ang natukoy na response gaps.
- Gumamit ng mitigation planning na may tatlong operational priorities: communication, coordination, at collaboration.
- Ipatupad ang response actions para sa lifesaving treatment, basic-needs access, at mabilis na referral sa shelter/resource systems.
- Sa active response, suportahan ang command-center communication, emergency-shelter operations, evacuation coordination, at rapid triage para sa displaced/high-risk populations.
- Isama ang weather at hazard intelligence mula sa authoritative public alerts sa staffing, evacuation, at shelter-in-place decisions.
- Ipatupad nang pare-pareho ang standardized mass-casualty triage systems (halimbawa START at pediatric JumpSTART) at muling suriin ang categories habang nagbabago ang kondisyon o resource availability.
- Gamitin ang mass-casualty tag priorities upang i-sequence ang care sa panahon ng scarcity (
REDimmediate life threat,YELLOWurgent major injury,GREENdelayed minor injury,BLACKexpectant/deceased). - Gumamit ng incident-command framework upang magtalaga ng malinaw na responsibilidad at mapabuti ang coordination sa mabilis na nagbabagong disaster response operations.
- I-activate nang maaga ang NIMS/ICS role structure sa MCI events upang ihanay ang interagency communication, resource tracking, at medical-branch triage-treatment-transport operations.
- Idirekta ang ambulatory casualties sa contamination screening at decontamination pathways bago ang unsupervised movement upang mabawasan ang secondary spread risk.
- Sa CBRN-risk incidents, isagawa ang zone-based operations: limitahan ang hot-zone entry, magsagawa ng decontamination/rapid triage sa warm zone, at maghatid ng treatment sa cold zone.
- I-activate ang surge-capacity plans sa pagbubukas ng karagdagang care areas, pagmomobilisa ng supplemental staffing, at muling paglalaan ng constrained resources.
- Sa infectious o mixed-hazard disasters, ipatupad ang containment operations gamit ang isolation precautions, PPE, environmental cleaning, at cohorting workflows.
- Magbigay ng psychological first-response actions: itaguyod ang safety, calm, connectedness, self-efficacy, at practical hope.
- Simulan ang decontamination protocols kapag naroon ang contamination indicators o kapag sinusuportahan ng protocol criteria ang precautionary decontamination.
- Gumamit ng hazard-specific interventions (halimbawa oxygenation support, antidote/chelation pathways, communicable-disease precautions, at mandatory reporting channels) ayon sa presentation.
- Sa infectious outbreaks, suportahan ang epidemiologic tracking, community screening/testing, vaccine operations, direct care delivery, at public prevention education.
- Sa biological-disaster response, mabilis na i-escalate ang infection-prevention measures (hand hygiene, PPE, isolation, at exposure follow-up) habang nakikipag-coordinate sa public-health reporting channels.
- Para sa suspected biologic mass exposure, ipatupad ang exposure-recognition workflow: limitahan ang karagdagang exposure, magtatag ng decontamination-treatment-clean zones, i-activate ang command chain, at triage/treat/transport casualties.
- Sa technological-disaster response, i-activate ang downtime communication/documentation plans, panatilihin ang medication/device safety controls, at ihiwalay ang compromised systems ayon sa cyber-incident policy.
- Makipag-coordinate sa public-health at emergency partners upang humiling ng Strategic National Stockpile/medical countermeasure support kapag kulang ang local critical assets.
- Sa epidemic/pandemic response, patibayin ang triage-screening entry workflows, agarang isolation para sa suspected cases, at tuloy-tuloy na community education sa hygiene, vaccination, at early-care seeking.
- Sa high-fatality respiratory outbreaks, i-deploy nang maaga ang nonpharmacologic control bundles at i-monitor ang consistency ng adherence sa iba’t ibang sites.
- Sa outbreak communication, isalin ang technical findings sa plain-language actions, aminin nang malinaw ang uncertainty, at ulitin ang updates sa trusted channels.
- Gumamit ng non-stigmatizing language at equity-centered outreach sa lahat ng pandemic messaging upang maiwasan ang avoidable exclusion mula testing, treatment, at follow-up care.
- Linawin nang maaga ang team communication roles at spokesperson responsibilities sa response operations upang mabawasan ang mixed messaging.
- Makipag-coordinate sa local/state/federal emergency structures kapag lumampas ang surge thresholds sa routine institutional capability.
- Bumuo ng culturally inclusive preparedness plans sa paggamit ng multilingual messaging, pag-angkop sa culturally linked dietary o mourning practices sa shelter workflows, at pakikipag-partner sa community leaders/organizations.
- Gumamit ng ongoing continuing education at rapid evidence updates (halimbawa PPE, transmission precautions, emerging therapeutics) upang mapanatili ang ligtas na response practice.
- Gumamit ng pre-event nurse preparedness checklists na naglilinaw ng alerts/warnings, employer role expectations, applicable state disaster obligations, travel-to-work contingencies, at family communication plans.
- Gamitin ang organization-specific evacuation routes at shelter locations, at isaalang-alang ang mobility-limited patients na hindi kayang mag-self-evacuate.
- Turuan ang high-risk patients/families na magpanatili ng handang emergency kit (essential medications, key documents, at basic supplies) para sa rapid displacement events.
- Suportahan ang recovery sa pamamagitan ng paulit-ulit na behavioral health surveillance, community resource linkage, at resilience-focused education.
Panganib ng Secondary Contamination
Ang naantalang isolation o decontamination ay maaaring makasama sa responders, staff, at ibang pasyente habang nakagagambala sa operations ng pasilidad.
Pharmacology
Exposure-dependent ang pharmacologic management sa disasters at maaaring kabilang ang oxygen therapy, antidotes, chelating agents, antimicrobials, sedatives para sa severe agitation, o seizure-control agents. Dapat nakaayon ang medication strategy sa triage priority at hazard-specific protocols.
Aplikasyon ng Clinical Judgment
Clinical Scenario
Pagkatapos ng isang chemical-release incident, ilang pasyente ang sabay-sabay na dumating na may respiratory symptoms, anxiety, at posibleng skin contamination.
- Recognize Cues: Maraming casualties, posibleng toxic exposure, at contamination risk sa staff at environment.
- Analyze Cues: Agarang priorities ang airway-breathing-circulation, contamination control, at triage categorization.
- Prioritize Hypotheses: Kabilang sa highest risk ang mabilis na respiratory decline at secondary contamination sa receiving area.
- Generate Solutions: I-activate ang disaster protocol, magtalaga ng triage categories, simulan ang decontamination pathway, at i-deploy ang behavioral support actions.
- Take Action: Ipatupad ang PPE-protected intake, hazard-specific treatment, at coordinated reporting/escalation.
- Evaluate Outcomes: Nagiging stable ang casualty flow, napipigilan ang secondary exposure, at natatanggap ng high-risk patients ang napapanahong definitive care.
Mga Kaugnay na Konsepto
- patient admission types, triage, at room readiness - Admission-level triage at throughput priorities sa routine at surge operations.
- individual at environmental safety sa nursing practice - Pagkilala sa environmental hazards at prevention-focused safety planning.
- safety data sheets at chemical hazard communication - Chemical hazard identification at exposure-response documentation.
- stress crisis staging at type-specific nursing response - Pamamahala sa crisis at behavioral response sa disaster-affected populations.
- Public Health Nursing - Community-level nursing coordination sa prevention, emergency response, at recovery.
Sariling Pagsusuri
- Bakit binabago ng social-vulnerability mapping ang disaster planning priorities?
- Aling findings ang dapat mag-trigger ng agarang decontamination precautions bago ang routine intake?
- Paano nagbabago ang behavioral health surveillance mula response phase hanggang recovery phase?