Balangkas ng Levels of Care na Primary Secondary at Tertiary
Mahahalagang Punto
- Binibigyang-diin ng primary care ang prevention, early identification, at routine management.
- Tinutugunan ng secondary care ang focused acute o specialty needs at pinapatatag ang patient status.
- Naghahatid ang tertiary care ng advanced diagnostics, invasive procedures, at major-surgery management para sa severe o highly complex conditions.
- Nangangailangan ang ligtas na care ng planadong paggalaw sa pagitan ng levels na may malinaw na referral at return-to-primary pathways.
- Maaaring pumasok ang mga pasyente sa secondary care kapag pinapabagal ng access barriers ang primary evaluation, na nagpapataas ng risk at cost.
- Ang primary, secondary, at tertiary prevention ay action levels na maaaring mangyari sa maraming care settings, hindi fixed facility tiers.
- Dapat mapanatili ng tertiary prevention para sa chronic illness ang function at quality of life sa pamamagitan ng rehabilitation, symptom control, at continuity follow-up.
Pisyopatolohiya
Ang levels of care ay kumakatawan sa healthcare delivery design, hindi biologic disease process. Gumagalaw ang mga pasyente sa pagitan ng levels batay sa complexity, acuity, at kinakailangang expertise.
Karaniwang nangyayari ang care failures sa transition points kapag hindi malinaw na naipapaliwanag ang referral intent, treatment goals, at follow-up responsibilities.
Klasipikasyon
- Primary care: Health promotion, prevention, screening, at routine chronic care.
- Primary care first-contact role: Karaniwang entry point para sa new concerns, annual exams, immunizations, at common mild-to-moderate problems.
- Primary care continuity role: Ongoing relationship sa paglipas ng panahon na sumusuporta sa early detection, reduced downstream cost, at mas ligtas na escalation kapag tumataas ang complexity.
- Primary care medical-home role: Comprehensive coordination hub na nag-uugnay ng specialty referrals at nagpapanatili ng quality/safety sa lahat ng levels.
- Primary care service breadth: Malawak na outpatient procedures/services (halimbawa basic lab testing, injections, x-rays, minor wound care, nutrition counseling, at chronic-condition follow-up).
- Primary care setting diversity: Offices, walk-in/urgent sites, pharmacies, school-based services, at community outreach settings.
- Secondary care: Specialist evaluation at management ng mas complex acute/chronic problems na may layuning stabilization, education, at return to baseline.
- Secondary care access pattern: Karaniwang referral-based ngunit maaari ring direct unscheduled entry sa pamamagitan ng emergency/urgent presentation.
- Secondary care clinical profile: Organ-focused, karaniwang noninvasive o minimally invasive services (halimbawa advanced imaging, specialty testing, same-day procedures, focused therapies, at crisis mental-health care).
- Tertiary care: Pinakamataas na complexity care para sa severe, rare, o multi-comorbidity conditions na nangangailangan ng highly specialized staff, advanced technology, at invasive o major procedural care.
- Secondary-tertiary provider overlap: Maaaring mag-overlap ang disciplines, ngunit may karagdagang advanced management scope ang tertiary providers (halimbawa operative o critical-care specialization).
- Tertiary care availability pattern: Mas kaunti ang facilities kaysa secondary care, kadalasang nasa malalaking urban o specialty centers na may transport mula sa ibang sites kapag kailangan.
- Tertiary care treatment arc: Karaniwang specific at time-bounded sa paligid ng severe events; ibinabalik ang care sa secondary/primary teams pagkatapos ng stabilization o definitive treatment.
- Tertiary setting spectrum: Karaniwan ang Level 1 trauma at specialty hospitals, ngunit maaari ring mangyari ang tertiary intensity sa specialized outpatient programs kapag mataas ang team expertise at intensity.
- Transition pattern: Escalation para sa complexity, pagkatapos de-escalation pabalik sa continuity care.
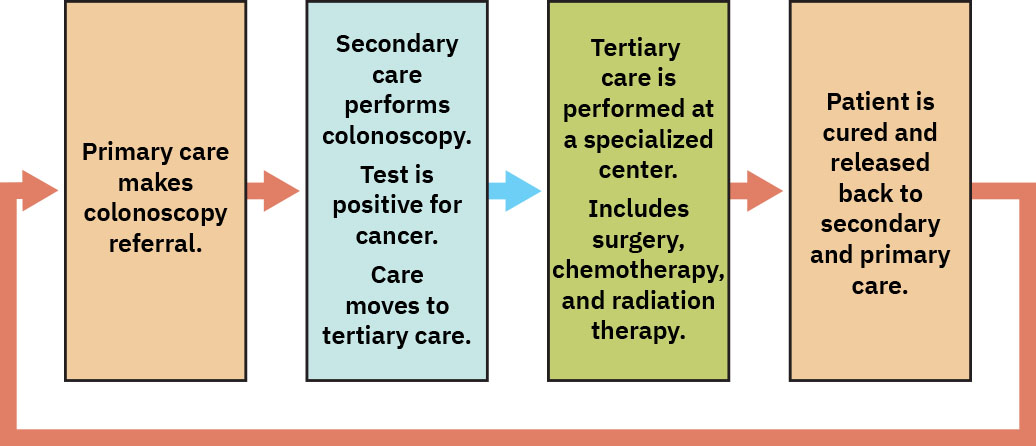 Illustration reference: OpenStax Fundamentals of Nursing Ch.3.1.
Illustration reference: OpenStax Fundamentals of Nursing Ch.3.1.
- Prevention-versus-care distinction: Ang primary/secondary/tertiary prevention ay action levels at hindi katumbas ng primary/secondary/tertiary care settings; maaaring maibigay ang tertiary prevention sa primary care.
- Primary-prevention action domain: Disease-before-onset prevention sa pamamagitan ng immunization, healthy-lifestyle support, at injury-risk reduction.
- Secondary-prevention action domain: Early detection at early treatment sa pamamagitan ng screening at napapanahong intervention.
- Tertiary-prevention action domain: Ongoing disease-impact reduction sa pamamagitan ng chronic-care management, rehabilitation services, symptom-control treatment, at scheduled follow-up pagkatapos ng diagnosis.
Pagsusuri sa Pag-aalaga
Pokus sa NCLEX
I-prioritize kung saan dapat makatanggap ng care ang pasyente ngayon at anong transition details ang kailangan para sa safety.
- Suriin ang kasalukuyang acuity, stability, at urgency upang matukoy ang care-level fit.
- Suriin kung kayang ibigay ng kasalukuyang setting ang kinakailangang diagnostics/interventions.
- Suriin ang referral indications at urgency para sa specialist o tertiary services.
- Suriin ang discharge/readiness factors para sa pagbabalik sa mas mababang level na may follow-up.
- Suriin ang pag-unawa ng pasyente kung bakit nangyayari ang transitions.
- Suriin kung may reliable primary-care attachment ang pasyente; pinapataas ng kawalan ng PCP linkage ang late at higher-acuity entry risk.
- Suriin ang access barriers (transportation, appointment availability, insurance/coverage, rural availability, fear/delay) na maaaring maglipat ng entry mula primary patungong secondary care.
- Suriin kung lumalampas sa secondary capability ang kinakailangang intervention (halimbawa major surgery, advanced subspecialty diagnostics, o intensive multi-comorbidity management) at dahil dito ay nangangailangan ng tertiary transfer.
- Suriin ang medication-fragmentation risk kapag maraming specialists ang aktibo, lalo na sa older adults na may multimorbidity.
Mga Interbensyon sa Pag-aalaga
- I-coordinate ang napapanahong referrals na may kumpletong clinical context at rationale.
- Linawin ang goals ng bawat level at inaasahang handoff outcomes.
- Turuan ang patient/family kung saan hihingi ng routine vs urgent vs specialized care.
- Linawin na maaaring magkaiba sa iisang encounter ang prevention action level at care delivery level.
- Ituro ang konkretong prevention examples ayon sa level (primary: immunization/lifestyle risk reduction; secondary: screening at early treatment; tertiary: rehab/chronic-condition self-management support).
- Sa secondary-prevention counseling, tukuyin ang age at risk triggers para sa screening escalation, kabilang ang mas maagang schedules kapag may family-history o genetic risk.
- Kumpirmahin ang return pathway sa primary care pagkatapos ng specialty episodes.
- Idokumento ang transition decisions at contingency instructions.
- Patibayin ang primary-care access points lampas sa physician offices (halimbawa walk-in clinics, urgent care, pharmacies, at school-based services) kapag naaangkop.
- I-frame ang secondary referrals bilang time-limited problem-focused episodes kapag clinically appropriate, at tukuyin ang follow-up ownership kapag nagta-transition pabalik sa PCP ang care.
- Para sa tertiary escalation, simulan ang rapid transfer logistics, malinaw na ipaalam ang severity risk, at magbigay ng family updates habang nagpaplano ng transport.
- I-predefine ang post-tertiary handback plans (secondary specialty follow-up plus primary continuity) bago discharge mula sa high-complexity centers.
- Kapag na-diagnose ang chronic disease, i-coordinate nang maaga ang tertiary-prevention services (halimbawa PT, OT, medication/symptom follow-up, at function-preservation planning) bago discharge.
- Gumamit ng PCP-led medical-home model para sa mga pasyenteng may maraming chronic conditions upang maisentralisa ang medication review at mabawasan ang cross-specialty treatment conflicts.
Transition Fragmentation
Ang pag-escalate ng care nang walang malinaw na return at follow-up plan ay nagpapataas ng readmission at missed-care risk.
Parmakolohiya
Madalas magbago ang medication regimens sa panahon ng secondary/tertiary episodes; mahalaga ang reconciliation at malinaw na post-transition instructions bago bumalik sa primary care.
Paglalapat ng Klinikal na Paghuhusga
Klinikal na Sitwasyon
Ang pasyenteng nakita sa primary care para sa lumalalang dyspnea ay nangangailangan ng urgent specialist intervention at posibleng procedural management.
- Recognize Cues: Lumalampas ang sintomas sa routine management threshold.
- Analyze Cues: Kailangan ang secondary o tertiary resources para sa definitive workup/treatment.
- Prioritize Hypotheses: Prayoridad ang agarang ligtas na escalation.
- Generate Solutions: Ayusin ang urgent referral at ipaalam ang risk details sa receiving team.
- Take Action: I-transfer na may kumpletong handoff at stabilization steps.
- Evaluate Outcomes: Naibibigay ang specialized care, pagkatapos ay naiuugnay muli ang follow-up sa primary care.
Mga Kaugnay na Konsepto
- patient care coordination, interdisciplinary referrals, at case management - Operational pathway para sa transitions.
- continuity of care sa evaluation phase - Tinitiyak ang stable follow-through pagkatapos ng level changes.
- nurse licensure compact at multistate practice - Relevant kapag tumatawid sa jurisdictions ang care transitions.
Sariling Pagsusuri
- Anong clinical factors ang pinakamatinding tumutukoy sa escalation mula primary patungong secondary care?
- Bakit dapat may malinaw na return-to-primary planning ang tertiary episodes?
- Aling handoff elements ang pumipigil sa avoidable transition-related harm?