Pagkilala sa Karaniwang Musculoskeletal Disorder at mga Prayoridad sa Pangangalaga
Mahahalagang Punto
- Kabilang sa mga karaniwang disorder ang spinal alignment abnormalities, inflammatory/degenerative joint disease, tendon disorders, at foot deformities.
- Ang maagang pattern recognition ay sumusuporta sa functional preservation at pag-iwas sa maiiwasang disability.
- Ang severe neurologic deficits, acute ischemic signs, o mabilis na functional decline ay nangangailangan ng agarang escalation.
Patopisyolohiya
Ang musculoskeletal disorders ay nagmumula sa congenital variation, repetitive mechanical stress, inflammatory o autoimmune processes, trauma, metabolic imbalance, at aging-related degeneration. Binabago ng mga mekanismong ito ang alignment, load transfer, at joint function.
Ang tuloy-tuloy na pamamaga at structural breakdown ay maaaring umusad mula sa sakit at paninigas tungo sa deformity, mobility loss, at pagbaba ng ADL independence.
Maaaring baguhin ng spinal disorders ang normal curve mechanics na sumusuporta sa upright posture at shock dissipation. Habang lumalala ang alignment, maaaring tumaas ang compensatory muscle/posture patterns na nagdudulot ng pagkapagod, sakit, neurologic symptoms (halimbawa paresthesia/panghihina), at dependency sa pang-araw-araw na gawain.
Pag-uuri
- Spinal disorders: Flatback syndrome, hyperlordosis, kyphosis, scoliosis, at ankylosing spondylitis patterns.
- Flatback pattern context: Ang pagkawala ng normal lumbar lordosis ay maaaring magdulot ng compensatory hip/cervical extension at knee flexion na may progresibong end-of-day fatigue at pain; kabilang sa etiologies ang nakaraang spinal surgery, congenital variation, degeneration, trauma, osteoporosis, at compression-fracture history.
- Bone-alignment disorders: Fracture/dislocation malalignment, intoeing, piling growth-plate disorders (halimbawa Blount disease), at accessory-bone variants na maaaring magbago ng gait/load distribution.
- Joint and bone disorders: osteoarthritis-degenerative joint disease, rheumatoid arthritis-autoimmune joint disease, at osteoporosis-bone density loss and fragility fracture risk.
- Traumatic bone disorders: Mga fracture pattern na nangangailangan ng reduction, immobilization, at neurovascular surveillance.
- Bone-shape/structure disorders: Degenerative spurring, cystic change, post-surgical structural variation, at neoplastic/metastatic reshaping.
- Bone-length discrepancy disorders: Congenital, infectious, traumatic, o neoplastic growth effects na nagdudulot ng clinically meaningful na pagkakaiba sa haba ng paa o kamay.
- Neoplastic bone disorders: Primary bone malignancies (osteosarcoma, Ewing sarcoma, chondrosarcoma) at metastatic bone involvement.
- Neurodevelopmental movement disorders: Cerebral palsy patterns na may spasticity, dyskinesia, o ataxia na nagbabago ng pangmatagalang mobility needs.
- Wrist-hand disorders: Ganglion cyst, tenosynovitis, at carpal tunnel syndrome.
- Foot-toe disorders: gout, pes planus, hallux valgus, at hammertoe.
Karagdagang Disorder Snapshots
- Ankylosing spondylitis: Inflammatory axial-spine disease na madalas lumalabas bilang chronic, gradual-onset back pain bago edad 40 na bumubuti sa activity at maaaring lumala sa gabi; agarang i-monitor para sa spinal-cord compression o cauda-equina pattern (bagong pamamanhid/panghihina ng extremity, pagkawala ng koordinasyon, foot drop, o bagong bowel/bladder dysfunction).
- Bone cancer: Pag-isipan kapag may persistent bone pain/swelling, pathologic-fracture tendency, fatigue, at unintended weight loss; maaaring kabilang sa workup ang X-ray, CT/MRI, PET, bone scan, at biopsy na may paggamot batay sa stage/type.
- Cerebral palsy: Nonprogressive brain injury/development disorder na nagdudulot ng persistent movement/posture impairment (spasticity, dyskinesia, o ataxia) at nangangailangan ng individualized na pangmatagalang multidisciplinary support.
- Clubfoot (congenital talipes): Congenital inward/downward foot-position deformity na ginagamot nang maaga gamit ang serial casting; sa severe cases maaaring kailanganin ang surgery na sinusundan ng matagal na brace support.
- Dislocation/subluxation: Ang kumpleto o bahagyang joint displacement ay nagpapakita ng severe pain, pamamaga, deformity, at movement loss; nangangailangan ng agarang reduction at post-reduction stabilization/rehabilitation, na may mataas na recurrence risk.
- Fibromyalgia: Central pain-processing sensitivity disorder na may widespread pain, fatigue, sleep/cognitive symptoms, at mood comorbidity; multimodal ang management (exercise, education, stress/sleep optimization, at piling medications/CBT).
- Foot drop: Kawalan ng kakayahang mag-dorsiflex ng paa dahil sa neuromuscular weakness/paralysis; karaniwan ang gait compensation, at madalas gumagamit ang paggamot ng AFO-style bracing kasama ang gait-strengthening therapy.
- Ganglion cyst: Fluid-filled cyst na kadalasang nasa dorsal wrist sa ibabaw ng tendon sheath o joint; karaniwan sa kababaihan, sa mga taong humigit-kumulang 15-40 taong gulang, at sa repetitive wrist-load groups (halimbawa gymnastic activity). May ilang kusang bumubuti sa rest/splinting; maaaring magbigay-lunas sa sakit ang aspiration ngunit karaniwan ang recurrence, at ang persistent symptomatic cases ay maaaring mangailangan ng surgical excision.
- Gout: Inflammatory crystal arthropathy mula sa hyperuricemia (urate crystal deposition), karaniwang may recurrent flares sa great toe/lower limb; kadalasang kasama sa paggamot ang NSAIDs/colchicine para sa flares at allopurinol para sa recurrent hyperuricemia control.
- Osteomyelitis: Bone infection mula sa hematogenous spread, contiguous tissue spread, o direct inoculation; tumataas ang panganib kapag may diabetes/foot-ulcer at smoking comorbidity, at kadalasang nangangailangan ang paggamot ng prolonged IV antibiotics na may posibleng surgery.
- Osteoarthritis (DJD): Age-related degenerative joint disease mula sa repetitive inflammation-cartilage loss cycles, kadalasang nakaaapekto sa weight-bearing joints (spine/hips/knees) at pati sa fingers; tumataas ang panganib sa obesity, family history, at prior overuse/injury, na mas mataas ang prevalence sa kababaihan pagkatapos ng humigit-kumulang edad 50.
- Osteoporosis: Progresibong bone-density loss na nagdudulot ng fragility-fracture risk (lalo na sa hip, spine, at wrist); binibigyang-diin ng prevention at care ang calcium/vitamin D intake, weight-bearing activity, pag-iwas sa paninigarilyo, at medication therapy (halimbawa bisphosphonate/calcitonin contexts) kapag mataas ang fracture risk.
- Muscular dystrophy (kabilang ang DMD): Bihirang minanang progressive muscle disorders na may higit sa 30 subtypes at malawak na pagkakaiba sa onset/severity; karaniwang pangmatagalang trajectories ang mobility loss, contracture risk, scoliosis-related pulmonary decline, at kalaunang dependence sa paglalakad/ADLs na nangangailangan ng multidisciplinary care.
- Paralysis syndromes: Kabilang sa pattern-based distribution ang hemiplegia, paraplegia, at tetraplegia, na may flaccid vs spastic muscle effects; binibigyang-diin ng pangmatagalang care ang rehabilitation services at adaptive/assistive technology para sa independence.
- Pes planus (flat feet): Pagkawala ng medial longitudinal foot arch; karaniwan sa early childhood bago buo ang arch development at nauugnay sa kalaunang buhay sa obesity, posterior tibial tendon dysfunction, o tight Achilles/calf structures. Kabilang sa findings ang weight-bearing arch collapse, altered gait, at back/leg/ankle/foot pain. Maaaring kabilang sa management ang NSAIDs, orthotics, motion-control footwear, weight reduction support, at surgery para sa refractory severe deformity.
- Hallux valgus (bunion): Medial bony protrusion sa first metatarsophalangeal joint na may progresibong paglihis paloob ng great toe patungo sa katabing toes; nauugnay sa hereditary patterns, autoimmune/inflammatory joint disease contexts (halimbawa RA), at chronic tight-restrictive footwear. Karaniwang findings ang deformity na may erythema/edema, callus burden, sakit o pamamanhid, at hirap maglakad; kabilang sa management ang NSAIDs, ice, orthotics, footwear adjustment, PT, piling steroid injection, at bunionectomy sa severe cases.
- Hammertoe: Flexion deformity sa proximal interphalangeal region (madalas second toe) na may hammer-like contour; nauugnay sa trauma, hallux valgus, arthritis, congenital variants, at poor shoe fit, na may mas mataas na prevalence sa kababaihan. Karaniwang clinical cues ang corn/callus formation at masakit na gait. Ang maagang PT-guided exercises na may taping/splinting ay maaaring magpabagal ng pag-usad tungo sa fixed deformity; maaaring kabilang sa symptom relief ang intermittent ice, NSAIDs, o piling corticosteroid injection, na may surgery para sa refractory deformity.
- rhabdomyolysis-muscle breakdown and acute kidney injury risk: Acute muscle-breakdown syndrome na may panganib ng myoglobin-mediated renal injury, na nangangailangan ng mabilis na fluid resuscitation at renal monitoring.
- mga pinsala sa soft tissue: Ang sprain/strain/contusion/tendinitis/bursitis patterns ay karaniwang mina-manage gamit ang maagang RICE, activity modification, at follow-up kapag naantala ang recovery.
- Tenosynovitis (kabilang ang De Quervain at trigger finger): Ang tendon-sheath inflammation ay maaaring sumunod sa overuse, autoimmune disease (halimbawa RA), o infection (kabilang ang skin-flora pathogens tulad ng S. aureus at MRSA). Ang De Quervain pattern ay nagdudulot ng thumb-side wrist pain sa grip/fist/turning motions at madalas gamutin gamit ang splinting, NSAIDs, activity modification, steroid injection, o sheath-release surgery. Ang stenosing tenosynovitis (trigger finger) ay nagdudulot ng locking/clicking ng flexed digit at mas karaniwan sa may diabetes at mas matandang edad.
- Vertebral-curvature disorders: Ang kyphosis, lordosis, at scoliosis ay binabago ang spinal alignment at pain/function risk; mula monitoring hanggang bracing o surgery ang management batay sa severity, progression risk, at neurologic impact.
- Scoliosis sa school-age/adolescence: Ang lateral spinal curvature ay maaaring magpakita ng asymmetric shoulder/hip height, scapular prominence, at rib-height asymmetry sa forward bend; kabilang sa evaluation ang spinal imaging, at mula observation hanggang bracing, PT, o surgery ang management batay sa growth status at curve severity.
- Hyperlordosis (swayback) pattern: Ang exaggerated lumbar curve na may anterior abdominal at posterior pelvic prominence ay maaaring magdulot ng neck/low-back pain; kabilang sa sanhi ang obesity, pagbubuntis, matagal na posture strain, paggamit ng high heel, core weakness, at piling neuromuscular o structural disorders.
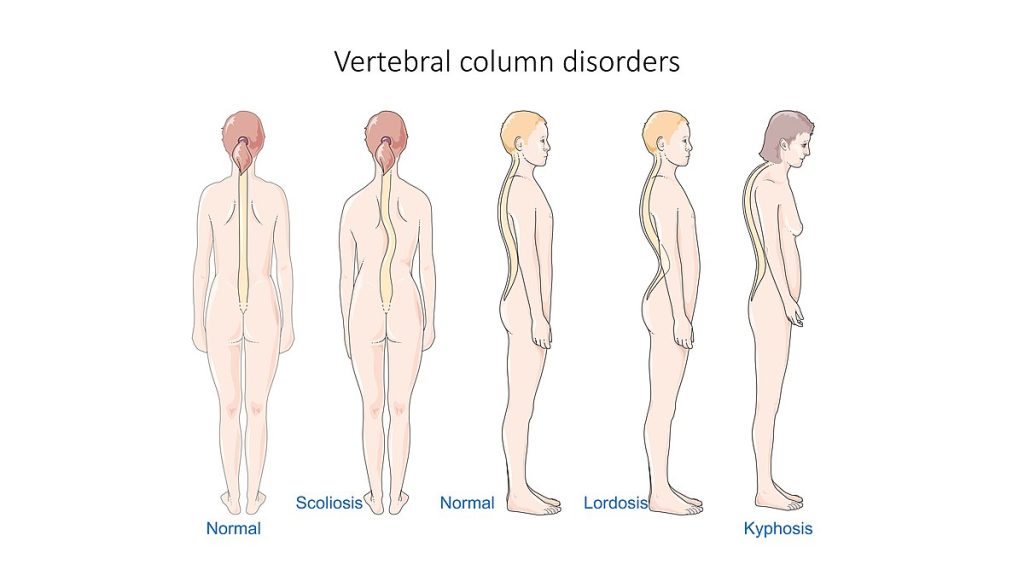 Sanggunian ng ilustrasyon: OpenRN Health Alterations Ch.10.10.
Sanggunian ng ilustrasyon: OpenRN Health Alterations Ch.10.10.
Nursing Assessment
Pokus sa NCLEX
Unahin ang mga sintomas na nagpapahiwatig ng nanganganib na neurologic function, severe inflammation, o mabilis na mobility decline.
- Tayahin ang pain pattern, stiffness, pamamaga, pag-usad ng deformity, at activity-related limitations.
- Sa chronic back-pain patterns, tasahin ang inflammatory features (mas batang onset, unti-unting chronicity, paglala sa gabi, at pagbuti sa paggalaw kaysa sa pahinga).
- Tayahin ang spinal posture at alignment changes kasama ang epekto sa gait at balanse.
- Tayahin ang hand/wrist sensory deficits, panghihina, at repetitive-use associations.
- Tayahin ang foot pain, joint erythema/heat, shoe-pressure effects, at weight-bearing tolerance.
- Agarang i-escalate ang bagong spinal-cord o cauda-equina cues (progresibong pamamanhid/panghihina ng extremity, foot drop, pagkawala ng koordinasyon, o bowel/bladder dysfunction).
Nursing Interventions
- I-escalate ang bagong neurologic deficits, bowel/bladder changes, severe inflammatory flare signs, o biglaang pagkawala ng function.
- Patibayin ang condition-specific self-management (activity modification, footwear support, at medication adherence).
- Patibayin ang DJD at osteoporosis self-management: low-impact activity, weight optimization, fall prevention, at pagsunod sa bone/joint medication plans.
- I-coordinate ang physical therapy, assistive-device planning, at follow-up para sa progressive disorders.
Panganib ng Hindi Na Mababawing Function-Loss
Ang naantalang pagtugon sa neurologic compromise, severe inflammation, o progresibong deformity ay maaaring magdulot ng permanent functional impairment.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| nsaids(mga NSAID) | Ibuprofen, naproxen contexts | Karaniwang ginagamit sa inflammatory pain; i-monitor ang response at adverse effects. |
| disease-modifying-antirheumatic-drugs(mga disease-modifying antirheumatic drug) | Methotrexate-class contexts | Ginagamit sa rheumatoid arthritis pathways; i-monitor para sa toxicity at infection risk. |
Paglalapat ng Klinikal na Paghuhusga
Klinikal na Sitwasyon
Ang pasyenteng may chronic back stiffness ay nagkaroon ng bagong pamamanhid sa binti at lumalalang gait instability.
- Kilalanin ang mga Palatandaan: Progresibong neurologic deficits na may functional deterioration.
- Suriin ang mga Palatandaan: Maaaring magpahiwatig ang pattern ng makabuluhang spinal involvement na nangangailangan ng agarang workup.
- Unahin ang mga Hinuha: Ang pag-iwas sa neurologic injury at pagpapanatili ng mobility ang agarang prayoridad.
- Bumuo ng mga Solusyon: Simulan ang agarang escalation at safety-focused mobility support.
- Kumilos: Idokumento ang objective deficits at i-activate ang angkop na referral pathway.
- Suriin ang Kinalabasan: Nililimitahan ng maagang interbensyon ang paglala at sinusuportahan ang recovery planning.
Mga Kaugnay na Konsepto
- musculoskeletal system - Structural at functional baseline para sa interpretasyon ng disorder.
- osteomyelitis - Pagkilala sa bone infection, diagnostics, at prolonged-treatment priorities.
- osteoarthritis-degenerative joint disease - Pag-usad ng degenerative joint disease, diagnostics, at treatment pathways.
- musculoskeletal physical assessment at functional mobility - Assessment sequence at red-flag detection.
- fracture - Type-based fracture recognition, komplikasyon, at treatment pathway.
- osteoporosis-bone density loss and fragility fracture risk - Pattern ng bone-density loss at mga prayoridad sa pag-iwas sa fragility fracture.
- mga pinsala sa soft tissue - Pagtatasa ng sprain/strain/contusion/tendinitis/bursitis at RICE-centered care.
- carpal tunnel syndrome - Median-nerve compression pattern sa loob ng wrist-hand disorders.
- pagsusulong ng joint mobility at aktibidad - Function-preserving activity strategies.
- mga komplikasyon ng immobility - Panganib ng disability progression kapag bumababa ang paggalaw.
Sariling Pagsusuri
- Aling musculoskeletal findings ang dapat i-escalate bilang agarang neurologic risk?
- Paano nagkakaiba ang degenerative at autoimmune joint disorders sa progression patterns?
- Bakit mahalaga ang maagang functional-support planning sa lahat ng karaniwang musculoskeletal disorders?