Multiple Sclerosis
Mahahalagang Punto
- Ang Multiple Sclerosis ay isang chronic immune-mediated CNS disorder na nailalarawan ng progresibong demyelination at lesion formation.
- Pinakakaraniwang disabling neurologic disease sa younger adults, na madalas nade-diagnose sa edad 20 hanggang 40 years.
- Maaaring relapsing-remitting o progressive ang kurso, na may pabagu-bagong motor, sensory, visual, cognitive, at psychosocial effects.
- Karaniwang gumagamit ang acute relapse treatment ng short-course high-dose IV glucocorticoids; ang pangmatagalang disease control ay umaasa sa immune-modifying therapies.
- Nakatuon ang care priorities sa relapse control, function preservation, fatigue/heat management, at pag-iwas sa falls, skin injury, at social isolation.
- Ang adjunctive nutrition strategies (kabilang ang ketogenic-pattern trials) ay may limitado ngunit umuusbong na ebidensya para sa suporta sa cognitive at fatigue-related symptoms.
Patopisyolohiya
Ang MS ay pinapagana ng immune-mediated injury sa myelin at neural tissue sa utak at spinal cord. Ang demyelination ay nagpapabagal o humaharang sa impulse conduction, na nagdudulot ng deficits sa mobility, sensation, coordination, at communication.
Maaaring kabilang sa maagang sakit ang partial remyelination na may pansamantalang pagbuti ng sintomas, ngunit ang paulit-ulit na lesion formation ay humahantong sa cumulative neuronal injury, cortical atrophy, at progresibong disability.
Pag-uuri
- Relapsing-remitting MS: Episodic exacerbations na may partial o complete remission; pinakakaraniwang presentasyon.
- Primary progressive MS: Tuloy-tuloy na neurologic decline nang walang malinaw na remissions.
- Secondary progressive MS: Progresibong deterioration pagkatapos ng initial relapsing-remitting course.
- Progressive-relapsing MS: Patuloy na deterioration na may superimposed relapses at incomplete recovery.
Konteksto ng Panganib at Etiology
- Sentral sa disease mechanisms ang autoimmune dysfunction.
- Karaniwang epidemiologic patterns ang female sex at early-adult onset (madalas 20-40 years).
- Kabilang sa infectious associations ang naunang EBV exposure at iba pang viral triggers.
- Tumataas ang genetic susceptibility kapag may apektadong first-degree relatives.
- Ang mas mababang vitamin D status at paninirahan na mas malayo sa equator ay kaugnay na risk patterns.
- Pinapataas ng paninigarilyo ang panganib at inuugnay sa mas mabilis na disability progression.
Nursing Assessment
Pokus sa NCLEX
I-track ang progression pattern sa paglipas ng panahon at ihiwalay ang intermittent exacerbations mula sa persistent deterioration.
- Suriin ang symptom timeline (constant vs intermittent, worsening trend, remission pattern) at karaniwang aggravators tulad ng fatigue, stress, at temperature extremes.
- Suriin ang visual findings (unilateral vision loss, diplopia, nystagmus, patchy blindness) at communication changes (halimbawa dysarthria).
- Suriin ang optic-nerve inflammatory patterns (halimbawa painful vision loss) dahil maaaring biglang magpababa ng visual function ang demyelinating injury.
- Suriin ang motor/sensory at coordination findings: weakness, spasticity, ataxia, dysmetria, tremor, paresthesia/hypoesthesia, mobility tolerance, at dizziness-related imbalance.
- Suriin ang bowel/bladder at sexual-function changes, cognitive impairment, mood/anxiety/lability, at panganib ng social withdrawal.
- Suriin ang fatigue burden at epekto nito sa activity pacing, fall risk, at pagkumpleto ng self-care.
- Suriin ang diagnostics sa konteksto: pangunahing ginagamit ang blood testing upang i-exclude ang mimics (halimbawa Lyme disease) at tukuyin ang modifiable risk factors tulad ng vitamin D deficiency.
- Suriin nang magkasama ang CSF at neurodiagnostic findings: maaaring magpakita ang lumbar puncture ng MS-pattern antibody abnormalities habang sinusuportahan ng MRI lesions at delayed evoked potentials ang demyelinating conduction defects.
- Sa panahon ng immunomodulator therapy, suriin ang nutrition-linked adverse-effect cues tulad ng pagkawala ng gana, persistent nausea, dark urine, clay-colored stool, o jaundice na maaaring senyales ng hepatotoxicity.
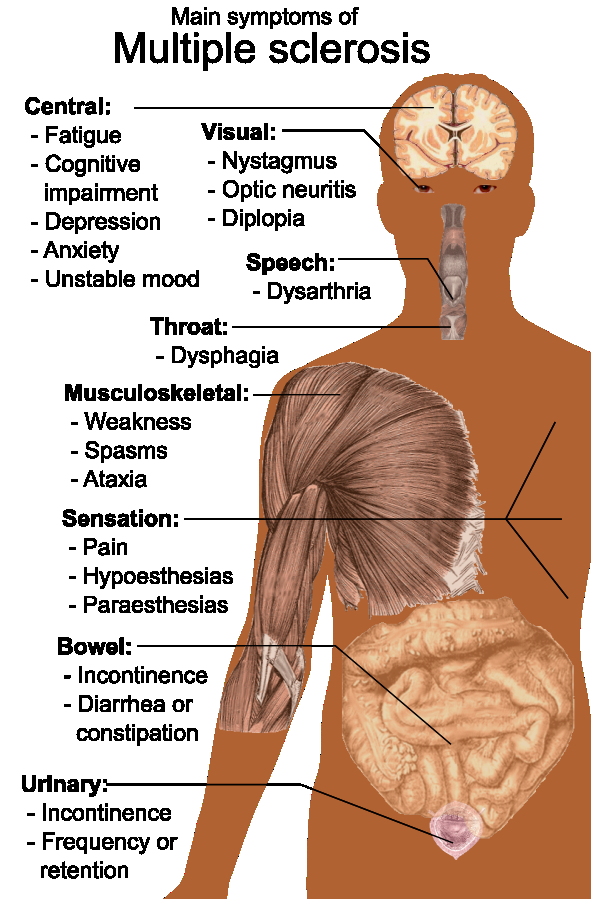 Illustration reference: OpenRN Health Alterations Ch.9.10.
Illustration reference: OpenRN Health Alterations Ch.9.10.
Nursing Interventions
- Hikayatin ang ligtas na independent activity at araw-araw na stretching/strengthening ayon sa tolerance.
- I-trend ang vital signs sa panahon ng exacerbations at habang nasa corticosteroid therapy; maaaring magpahiwatig ng treatment burden ang BP changes at sleep/mood shifts.
- Gumamit ng energy-conservation plans (activity clustering, planned rest, pag-aayos ng madalas gamitin na items).
- Ipatupad ang bowel/bladder training na may scheduled toileting at hydration support.
- Ilapat ang fall precautions at skin-protection measures, kabilang ang madalas na assessment para sa breakdown sa immobility/incontinence.
- Pamahalaan ang heat sensitivity (temperature control strategies at cooling aids kapag indikado) upang mabawasan ang pansamantalang paglala ng sintomas.
- Suportahan ang visual at communication adaptation (halimbawa alternating eye patch use para sa diplopia, therapy-guided communication strategies).
- I-monitor ang plasmapheresis sessions kapag iniutos, kabilang ang access-site status, infection prevention, at hemodynamic tolerance.
- I-coordinate ang physical therapy at behavioral-health support para sa gait/balance deficits at anxiety/depression coping.
- Kung pipili ang client ng therapeutic diet modification, i-coordinate ang dietitian-guided planning at i-monitor ang tolerance/adherence upang hindi magpalala ng fatigue o function ang nutritional deficits.
- I-escalate nang maaga ang persistent treatment-related nausea o intake decline upang maiwasan ang secondary malnutrition at dehydration sa panahon ng relapse-prevention therapy.
- Itaguyod ang pahinga, stress-management skills, at paglahok sa support groups upang mabawasan ang isolation at mapabuti ang coping.
Medical at Rehabilitation Management
- Karaniwang gumagamit ang disease-modifying management ng interferons, oral immunomodulators, mga monoclonal antibody, at S1P-receptor modulators; bantayan ang infection risk, organ toxicity, at class-specific cardiovascular o neuro-ophthalmic complications.
- Karaniwang unang ginagamot ang acute exacerbations gamit ang short-course high-dose IV glucocorticoids (halimbawa methylprednisolone); karaniwang next-line strategy ang plasmapheresis kapag hindi sapat ang steroid response.
- Maaaring isaalang-alang ang IV immune-globulin pathways sa piling refractory o steroid-intolerant contexts.
- Maaaring kabilang sa symptom-directed medications ang mga muscle relaxant para sa spasticity, anticonvulsant o tricyclic options para sa paresthesia-related pain, bowel-regimen agents, at bladder-relaxing medications.
- Sentral ang PT/OT/ST sa mobility, ADL adaptation, visual-scanning strategies, at communication/swallow support.
- Sa severe refractory tremor, maaaring isaalang-alang ang neurosurgical options (kabilang ang deep-brain stimulation contexts).
Panganib ng Functional Decline at Kaligtasan
Ang hindi makontrol na fatigue, progresibong panghihina, heat-triggered symptom worsening, at falls ay maaaring mabilis na magpababa ng independence at quality of life.
Pharmacology
| Medication Context | Examples | Key Nursing Considerations |
|---|---|---|
| Acute relapse therapy | IV methylprednisolone high-dose short course; IV gamma globulin context | Bantayan ang glucose, mood, infection risk, at tugon sa relapse treatment. |
| Interferon pathway therapy | interferon beta-1a, interferon beta-1b | Bantayan ang CBC/LFT/thyroid trends, injection-site injury, mood o suicidality, at flu-like symptoms. |
| Oral immunomodulators | teriflunomide, monomethyl fumarate, glatiramer acetate | I-screen ang TB/pregnancy risk, bantayan ang hepatotoxicity at BP, iwasan ang live vaccines, at palakasin ang barrier contraception kapag indikado. |
| Monoclonal antibody therapy | ocrelizumab, natalizumab, alemtuzumab | Gumamit ng infusion-reaction precautions na may premedication, bantayan ang infection/PML at autoimmune toxicity, at sundin ang restricted-program monitoring requirements kung naaangkop. |
| S1P-receptor modulators | siponimod pathway | Kailangan ang baseline ECG/labs at first-dose bradycardia monitoring; tiyakin ang CYP2C9 genotype bago ang siponimod at bantayan ang mga senyales ng macular edema, PRES, at skin malignancy. |
| Spasticity and symptom control | baclofen-class at dantrolene contexts | Suriin ang tone, sedation, fall risk, withdrawal safety, at panganib ng liver toxicity sa dantrolene. |
| Neuropathic/sensory symptom control | anticonvulsant o tricyclic contexts (halimbawa gabapentin/pregabalin) | Bantayan ang functional response, cognition, edema/weight changes, at abrupt-stop withdrawal risk. |
| Fatigue symptom control | modafinil, methylphenidate contexts | Muling suriin ang sleep quality, gana, HR/BP response, at daytime function sa stimulant-class therapy. |
| Bowel/bladder symptom programs | stool-softener/laxative at bladder-relaxant contexts | Bantayan ang elimination pattern, retention risk, at hydration status. |
Health Teaching and Evaluation
- Ituro ang layunin ng gamot, side effects, at kung kailan tatawag sa provider para sa adverse effects o relapse concerns.
- Ituro ang adaptive self-care skills, paggamit ng equipment, skin care, bowel/bladder routines, at home-safety modifications.
- Palakasin ang smoking cessation at risk-reduction habits na maaaring magpabagal ng disability progression.
- Isama ang family/caregivers sa education at iugnay sa counseling/community support services.
- Muling suriin ang outcomes sa bawat reassessment at i-revise ang plans kapag nagbago ang symptom pattern o functional status.
Clinical Judgment Application
Clinical Scenario
Ang client na may relapsing-remitting MS ay nag-uulat ng lumalalang afternoon fatigue, mas madalas na pagkatisod, urinary urgency, at bagong social withdrawal sa panahon ng mainit na summer period.
- Recognize Cues: Heat-linked symptom worsening na may mobility at psychosocial decline.
- Analyze Cues: Binabawasan ng exacerbation risk at fatigue burden ang kaligtasan at participation.
- Prioritize Hypotheses: Ang agarang prayoridad ay fall prevention, function support, at symptom-trigger reduction.
- Generate Solutions: Simulan ang energy-conservation plan, heat-mitigation strategies, bladder routine support, at therapy/social-support referrals.
- Take Action: Ipatupad ang safety interventions, palakasin ang teaching, at i-coordinate ang multidisciplinary follow-up.
- Evaluate Outcomes: Bumababa ang falls, mas nakokontrol ang fatigue, at bumubuti ang participation sa daily activities.
Mga Kaugnay na Konsepto
- neurological system - Mga pundasyon ng myelin at impulse transmission para sa MS pathology.
- pagkilala sa karaniwang neurological disorders at prayoridad na pangangalaga - Konteksto ng pattern recognition at escalation.
- mga prayoridad sa nursing care para sa neuromuscular impairment - Overlap sa mobility, aspiration, elimination, at skin risk.
- mga muscle relaxant - Konteksto ng spasticity-focused pharmacologic management.
- pag-iwas sa pagkahulog - Pangunahing safety framework para sa gait at coordination impairment.
Sariling Pagsusuri
- Aling findings ang nagmumungkahi ng progression versus remission sa MS symptom patterns?
- Paano binabago ng fatigue at heat sensitivity ang nursing care priorities?
- Aling interdisciplinary strategies ang pinakamahusay na nagpapanatili ng mobility at independence?