Malignant na Reproductive Neoplasms
Mahahalagang Punto
- Sentral sa pinahusay na outcomes sa gynecologic cancer care ang maagang detection at prevention.
- Kabilang sa pangunahing cancers sa domain na ito ang cervical, ovarian, uterine/endometrial, vulvar, at vaginal malignancies.
- Nagkakaiba ang risk, symptom pattern, at diagnostic approach ayon sa cancer site, ngunit nagpapalala ng prognosis ang delayed recognition.
- Saklaw ng nursing roles ang screening education, diagnostic/procedural support, symptom surveillance, at psychosocial care.
Patopisyolohiya
Nabubuo ang malignant neoplasms sa reproductive tissues sa pamamagitan ng progresibong cellular dysplasia at invasive transformation na may potensyal na metastasis. Malakas ang ugnay ng cervical malignancy sa oncogenic HPV strains, kaya sinusuportahan nito ang preventive role ng vaccination at guideline-based screening. Naiimpluwensiyahan ang endometrial at uterine malignancies ng prolonged unopposed estrogen exposure patterns.
Madalas na may nonspecific symptoms ang ovarian cancer at kadalasang nade-diagnose sa mas huling stages. Hindi gaanong karaniwan ang vulvar at vaginal cancers ngunit nangangailangan ng agarang evaluation ng persistent lesions, burning, bleeding, o nonhealing sores.
Gumagamit ang clinical screening follow-up ng cervical precancer continuum language (halimbawa LSIL, HSIL, adenocarcinoma in situ) at colposcopy/biopsy pathways kapag abnormal ang cytology. Nanatiling pangunahing warning sign para sa endometrial pathology ang postmenopausal bleeding na nangangailangan ng agarang transvaginal imaging at endometrial sampling. Para sa ovarian-risk counseling, madalas talakayin ang protective associations para sa prior anovulation-focused contraceptive use, breastfeeding history, at multiparity, habang ang persistent symptom clusters ay nangangailangan pa rin ng agarang evaluation.
Nakadepende sa site at stage ang management at maaaring kabilang ang surgery, radiation, chemotherapy, o multimodal treatment. Mahalaga ang nursing surveillance para sa treatment complications at emotional burden sa buong care continuum.
Klasipikasyon
- Cervical malignancies: HPV-associated dysplasia-to-cancer continuum.
- Uterine/endometrial malignancies: Hormone-linked endometrial pathology at uterine sarcoma variants.
- Ovarian malignancies: Madalas na advanced-stage presentations na may malawak na peritoneal involvement potential.
- Ovarian-stage framework: Stage I na limitado sa ovary/ovaries, Stage II pelvic extension, Stage III nodal o abdominal-lining spread, Stage IV distant metastasis (halimbawa liver o lung).
- Ovarian-screening limitation domain: Walang inirerekomendang routine mortality-reducing screening test para sa average-risk populations; suriin ang persistent unexplained symptom clusters at high-risk genetic/family history.
- Vulvar/vaginal malignancies: Mga bihirang cancer na may lesion-focused diagnostic pathways.
- Endometrial-screening domain: Hindi inirerekomenda ang routine asymptomatic screening; nangangailangan ng agarang endometrial evaluation ang postmenopausal o unexplained abnormal bleeding.
- Pregnancy-associated cancer-care domain: Maaaring mangailangan ang management ng pagbabalanse ng fetal maturity, maternal staging urgency, at ethically complex treatment-timing decisions.
- Breast malignancies: Ductal/lobular pathways na may lymphatic at hematogenous metastatic spread potential.
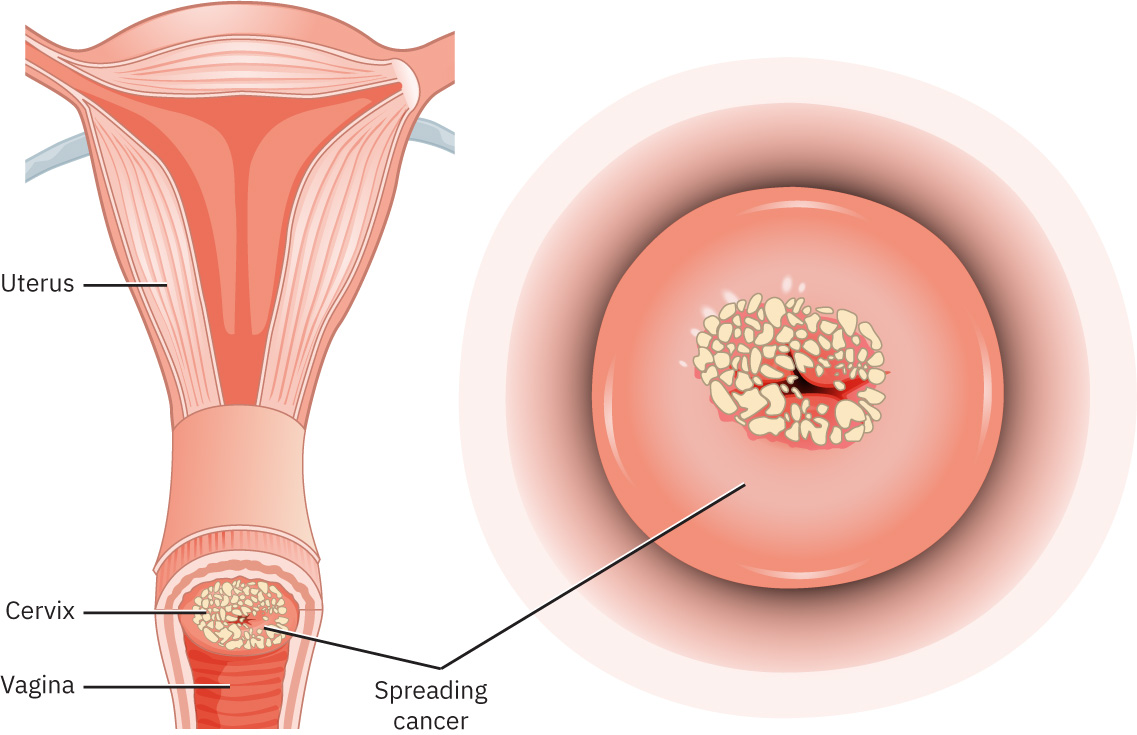 Illustration reference: OpenStax Maternal-Newborn Nursing Ch.6.4.
Illustration reference: OpenStax Maternal-Newborn Nursing Ch.6.4.
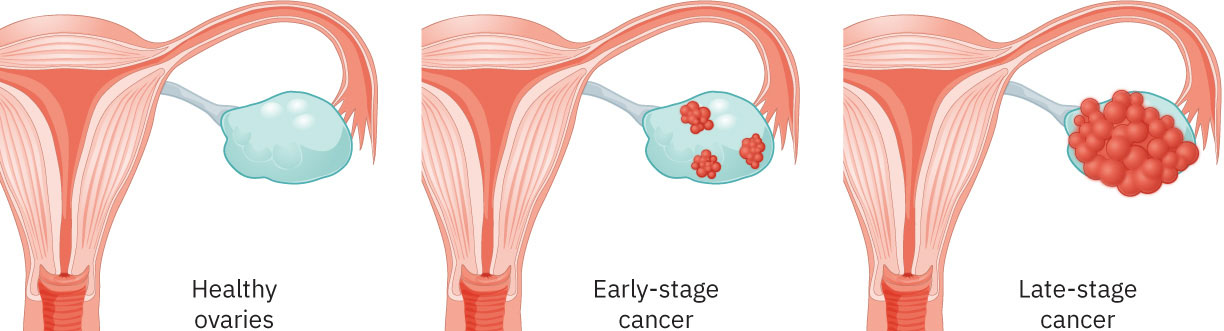 Illustration reference: OpenStax Maternal-Newborn Nursing Ch.6.4.
Illustration reference: OpenStax Maternal-Newborn Nursing Ch.6.4.
Pagtatasa sa Pag-aalaga
Pokus sa NCLEX
Unahin ang pagkilala sa high-risk symptoms (postcoital o postmenopausal bleeding, persistent pelvic pain, unexplained weight loss) at napapanahong diagnostic follow-through.
- Tayahin ang screening history (Pap/HPV co-testing at mga naunang abnormal results).
- I-verify ang applicability ng age- at surgery-context screening (halimbawa walang routine cervical screening bago ang age 21 at individualized discontinuation decisions pagkatapos ng 65 o pagkatapos ng hysterectomy kapag natugunan ang criteria).
- Suriin ang red-flag symptoms: abnormal bleeding, persistent discharge, pelvic pressure/pain, nonhealing vulvar lesions.
- Para sa vulvar/vaginal-risk concern, tasahin ang persistent itching o burning, nonhealing sore, wart-like growth, raised/discolored vulvar skin, changing mole, o groin-node swelling.
- Kung abnormal ang cervical screening, asahan ang ASCCP/Bethesda-guided stratification steps at kumpirmahin ang follow-up colposcopy/biopsy plans.
- Para sa ovarian-risk concern, tasahin ang persistent bloating, early satiety, urinary urgency/frequency, at unexplained bowel-pattern change.
- Isama ang ovarian-risk profile cues tulad ng obesity, nulliparity, infertility, endometriosis history, at mas mahabang lifetime estrogen exposure patterns.
- Isama ang cancer-site specific red flags: new breast/axillary lump o nipple change, postmenopausal bleeding, at persistent pelvic fullness/bloating.
- Kolektahin ang risk-profile cues (HPV exposure, smoking, immunocompromise, family/genetic risk factors).
- Para sa endometrial-risk contexts, tasahin ang obesity, PCOS history, at prolonged unopposed-estrogen exposure patterns.
- Tayahin ang treatment readiness, pag-unawa sa diagnostic steps, at psychosocial distress burden.
- I-monitor ang peri-procedural at treatment-related adverse effects (bleeding, infection, pain, fatigue).
Mga Interbensiyong Pang‑nars
- Magbigay ng evidence-based education tungkol sa cancer prevention, vaccination, at screening intervals.
- Linawin na maaaring magkaiba ang professional organizations sa detalye ng intervals; palakasin ang paggamit ng kasalukuyang local guideline at shared decision-making kapag magkakaiba ang recommendations.
- Ihanda ang mga pasyente para sa diagnostic procedures (Pap/HPV testing, colposcopy, biopsy, imaging) at postprocedure expectations.
- Palakasin ang postprocedure expectations pagkatapos ng colposcopy/LEEP/biopsy (posibleng light vaginal bleeding, paggamit ng peripad, return precautions, at malinaw na result-communication timeline).
- Pagkatapos ng endometrial/cervical biopsy, palakasin ang return precautions para sa heavy vaginal bleeding (halimbawa pagbasa ng pad humigit-kumulang bawat 1 to 2 hours), fever, o lumalalang abdominal pain.
- Sa high-risk ovarian contexts, ipaliwanag ang limitations ng CA-125 at transvaginal ultrasound bilang stand-alone screening tests at palakasin ang individualized surveillance planning.
- Palakasin ang agarang return precautions para sa heavy bleeding, fever, severe pain, o lumalalang systemic symptoms.
- Sa pregnancy-associated cancer contexts, suportahan ang informed discussions sa treatment timing options, maternal-fetal implications, at ethical support resources.
- I-coordinate ang interdisciplinary oncology care at supportive services para sa pasyente at pamilya.
- Maghatid ng trauma-informed at culturally sensitive communication sa panahon ng high-stress diagnosis at treatment decisions.
Vague-Symptom Dismissal
Ang pagtrato sa persistent abnormal bleeding o pelvic symptoms bilang benign nang walang napapanahong workup ay maaaring magpaantala ng diagnosis hanggang later-stage disease.
Farmakolohiya
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| breast-cancer-chemotherapy-safety-and-support(kaligtasan at suporta sa breast cancer chemotherapy) (chemotherapy) | Site- and stage-specific regimens | Nangangailangan ng adverse-effect monitoring, infection-prevention teaching, at symptom escalation planning. |
| sexual-history-risk-linking-and-preventive-counseling(pagtatasa ng sexual history, pag-uugnay ng risk, at preventive counseling) (hpv-vaccine) | Cervical/vulvovaginal cancer-prevention contexts | Core prevention strategy; palakasin ang eligibility, schedule completion, at screening continuation. |
Aplikasyon ng Clinical Judgment
Klinikal na Sitwasyon
Isang postmenopausal na pasyente ang nag-uulat ng intermittent bleeding at pelvic discomfort sa loob ng 2 months ngunit naantala ang pagpapatingin dahil “malamang stress-related lang” ang sintomas.
- Recognize Cues: High-priority malignancy warning sign ang postmenopausal bleeding.
- Analyze Cues: Pinapataas ng pagkaantala sa evaluation ang panganib ng later-stage diagnosis.
- Prioritize Hypotheses: Agarang prayoridad ang exclusion ng endometrial/uterine pathology sa pamamagitan ng pinadaling diagnostic workup.
- Generate Solutions: Ayusin ang urgent gynecologic assessment, biopsy pathway, at symptom support.
- Take Action: I-escalate para sa definitive testing at magbigay ng malinaw na follow-up safety instructions.
- Evaluate Outcomes: Naipapagtatag ang napapanahong diagnosis at nasisimulan ang stage-appropriate treatment.
Mga Kaugnay na Konsepto
- benign reproductive growths - Maaaring mag-overlap ang benign at malignant bleeding o mass symptoms at nangangailangan ng maingat na differentiation.
- mga structural reproductive disorder - Maaaring magsabay ang structural abnormalities at magkomplikado sa diagnostic interpretation.
- mga functional reproductive disorder - Hindi dapat matabunan ng functional bleeding patterns ang cancer warning signs.
- therapeutic communication - Nangangailangan ng malinaw, mahabagin, at culturally safe communication ang oncology conversations.
- culturally competent care - Nakadepende ang pantay na cancer care sa language access at context-sensitive counseling.
Self-Check
- Aling mga sintomas sa reproductive oncology ang dapat mag-trigger ng agarang diagnostic escalation?
- Bakit madalas na naipapakita ang ovarian cancer sa mas advanced na stages?
- Paano pinapabuti ng nursing education at screening outreach ang gynecologic cancer outcomes?