Seizures and Epilepsy
Mahahalagang Punto
- Ang seizure ay biglaan at hindi makontrol na neuronal discharge na maaaring magbago sa movement, sensation, behavior, at awareness.
- Ang epilepsy ay tinutukoy ng recurrent unprovoked seizures (hindi bababa sa dalawang events, may pagitan na hindi bababa sa 24 hours).
- Sa United States, naaapektuhan ng epilepsy ang milyun-milyong tao at maaaring lubhang magpababa ng quality of life kung walang tuloy-tuloy na management support.
- Ang status epilepticus (seizure >5 minutes o serial seizures na walang recovery) ay neurologic emergency.
- Ang priority nursing goals ay airway protection, injury prevention, trigger reduction, at medication adherence.
- Sa piling refractory epilepsy pathways, maaaring mabawasan ng ketogenic-style nutrition therapy ang seizure burden kapag pinamamahalaan kasama ng care team.
- Maaaring baguhin ng antiepileptic regimens ang micronutrient status, bone-health risk, appetite/weight pattern, at piling drug-food interactions.
- Sa advanced illness, nananatiling prayoridad ang seizure prevention at trauma reduction kahit comfort-focused ang goals of care.
Patopisyolohiya
Nabubuo ang seizures kapag hindi balanse ang excitatory at inhibitory signaling sa CNS, na madalas kinasasangkutan ng nabawasang GABA-mediated inhibition at/o abnormal electrical firing networks. Ang resultang surge ng synchronized activity ay maaaring magdulot ng focal o generalized neurologic manifestations.
Maaaring idiopathic ang etiology o secondary sa structural, metabolic, infectious, vascular, toxic, withdrawal, o traumatic processes. Ang postictal recovery ay maaaring mula sa agarang pagbabalik sa baseline hanggang sa matagal na fatigue, confusion, o weakness.
Pag-uuri
- Focal (partial) seizures: Nagsisimula sa isang cerebral hemisphere.
- Focal-onset aware seizures: Napananatili ang awareness; maaaring kabilang ang aura (halimbawa deja vu, kakaibang amoy, biglaang sakit), unilateral motor/sensory change, o autonomic symptoms.
- Focal-onset impaired-awareness seizures: Confusion o nabawasang awareness na may automatisms (halimbawa lip smacking, repetitive leg movements), posibleng wandering, at postictal amnesia.
- Generalized seizures: Bilateral hemispheric involvement.
- Generalized subtypes: absence, tonic, clonic, tonic-clonic, myoclonic, at atonic (mataas ang injury risk mula sa biglaang pagkawala ng tone).
- Unclassified seizures: Mixed-pattern o hindi malinaw na etiology, kabilang ang primary/idiopathic at secondary causes.
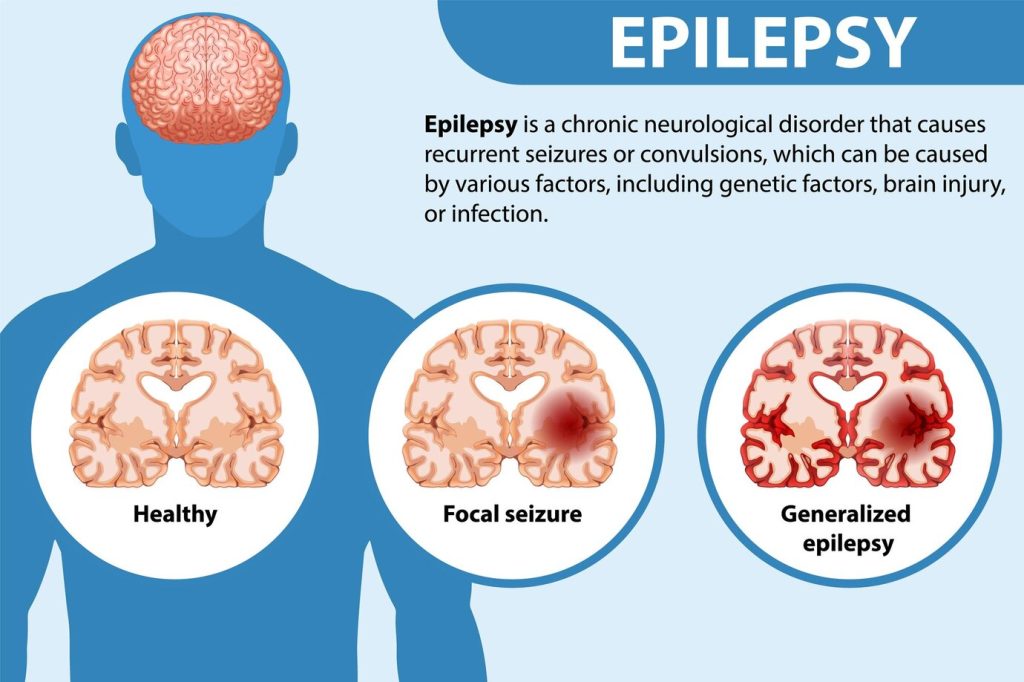 Illustration reference: OpenRN Mga Pagbabago sa Kalusugan Ch.9.7.
Illustration reference: OpenRN Mga Pagbabago sa Kalusugan Ch.9.7.
Mga Yugto at Trigger ng Seizure
- Phases: prodromal (preictal), aura, ictal, at postictal.
- Common triggers: stress, fatigue, sleep deprivation, alcohol/caffeine excess, dehydration o missed meals, hormonal fluctuation, flashing visual stimuli, toxins, at ilang medication/substance exposures.
- Nutrition-therapy context: Maaaring gamitin ang ketogenic o modified Atkins plans sa piling refractory epilepsy cases (mas karaniwan sa pediatrics) na may mahigpit na interdisciplinary monitoring.
Nursing Assessment
Pokus sa NCLEX
Sa panahon at agad pagkatapos ng seizure activity, ang unang prayoridad ay airway, oxygenation, at injury prevention.
- Kumuha ng detalyadong history: event count, duration, pattern, presensya ng aura, level of consciousness, at pre/during/post-seizure findings.
- Sa panahon ng active events, itala ang eksaktong onset at duration timing at kung bumabalik ang consciousness sa pagitan ng episodes upang mabilis na matukoy ang status-epilepticus risk.
- Suriin ang medication, supplement, alcohol, at substance-use context at comorbid neurologic/metabolic risk factors.
- Suriin ang medication-related nutrition effects (weight change, appetite shift, vitamin/mineral depletion, constipation, at bone-health risk).
- Suriin ang medication-access barriers (halimbawa cost/insurance loss) dahil karaniwan at maiiwasang trigger ng breakthrough seizures ang nonadherence.
- Suriin ang kamakailang medication toxicity/withdrawal risk at organ-failure-related metabolic imbalance bilang posibleng seizure precipitants.
- Suriin ang postictal airway safety, neuro status, agitation, orientation, at timing ng pagbabalik sa baseline.
- Sa school-age epilepsy care, suriin ang attendance disruption, learning-impact burden, at kahandaan ng school action plans/rescue-medication workflows.
- Gumamit ng diagnostics upang kumpirmahin ang pattern at i-rule out ang causes: EEG o SEEG, CT/MRI, SPECT/PET, lumbar puncture sa piling infectious contexts, at blood tests (electrolytes, CBC, glucose, toxicology, therapeutic drug levels tulad ng phenytoin/phenobarbital).
Nursing Interventions
- Kung may aura, ilipat ang client sa ligtas na pribadong lugar at protektahan mula sa environmental injury.
- Sa panahon ng seizure: huwag pigilan, huwag magpasok ng bagay sa bibig, protektahan ang ulo, luwagan ang masisikip na damit, alisin ang kalapit na hazards/glasses/neck items kung posible, at i-time ang event.
- Agad na i-escalate para sa status epilepticus at suportahan ang emergency response workflow.
- Pagkatapos ng seizure: side-lying recovery position, airway confirmation, vital signs/neuro checks, reorientation, kalmadong komunikasyon, at dokumentasyon ng presensya ng aura, onset time, active-duration time, at haba ng postictal recovery.
- Panatilihin ang inpatient seizure precautions kapag indikado (handang oxygen/suction equipment, bed sa low position, agency-based side-rail precautions).
- Suportahan ang psychosocial coping at family preparedness para sa recurrent-event management.
- Sa school settings, i-coordinate ang seizure action plans kasama ang caregivers, school nurse, teachers/coaches, at provider orders para sa rescue-medication availability.
- Magbigay ng seizure first-aid training at anti-stigma education support para sa school staff at peers upang mabawasan ang maiiwasang pinsala at social isolation.
- Kung inireseta ang ketogenic therapy, palakasin ang mahigpit na carbohydrate limits at tiyakin ang hidden sugar sources sa medications at supplements (halimbawa syrup formulations at gummy vitamins), dahil ang maliliit na sugar exposures ay maaaring magpababa ng therapeutic effect.
- Palakasin ang karaniwang antiepileptic interaction precautions: iwasan ang alcohol kasama ang anticonvulsants, paghiwalayin ang phenytoin sa enteral feedings, at repasuhin ang diet pattern issues (halimbawa mataas na soy intake sa valproate plans) kasama ang pharmacy/dietitian support.
Medical at Surgical Management
- Maaaring kabilang sa acute seizure control ang IV benzodiazepines (halimbawa lorazepam, diazepam, o midazolam), na may cardiorespiratory monitoring at airway support.
- Karaniwang gumagamit ang maintenance therapy ng antiepileptic drugs (halimbawa levetiracetam, phenytoin, phenobarbital), kasama ang fluid/electrolyte correction kapag indikado.
- Ang drug-resistant focal epilepsy ay maaaring mangailangan ng resective/disconnection procedures (halimbawa lobectomy, corpus callosotomy, hemispherotomy, multiple subpial transection, o thermal-ablation pathways) sa piling surgical candidates.
- Maaaring kabilang sa neuromodulation options ang vagal-nerve stimulation, responsive neurostimulation, o deep-brain stimulation sa piling refractory pathways.
High-Risk na Deterioration
Ang prolonged seizures ay maaaring magdulot ng neuronal injury, hypoxia, aspiration, at cardiorespiratory compromise kung maantala ang escalation.
Pharmacology
| Medication Context | Examples | Key Nursing Considerations |
|---|---|---|
| Acute seizure termination | IV lorazepam, diazepam, midazolam | Kailangan ang tuloy-tuloy na respiratory/cardiac monitoring at airway support. |
| Maintenance anticonvulsants | Levetiracetam, phenytoin, phenobarbital | Itugma ang gamot sa seizure type, bantayan ang adverse effects/toxicity, at palakasin ang mahigpit na adherence. |
| Titration and monitoring strategy | Monotherapy-first approach in many clients | I-titrate ang dose para sa seizure control/minimal toxicity; i-adjust para sa illness, stress, at weight changes. |
Hindi sinusuportahan ng kasalukuyang ebidensya ang routine anti-seizure medication initiation pagkatapos ng first-time seizure sa bawat client; inuuna ang mabilis na neurology follow-up at individualized risk discussion.
Health Teaching and Evaluation
- Ituro na huwag kailanman itigil bigla ang anticonvulsants at magbigay ng missed-dose instructions.
- Palakasin ang therapeutic-level lab follow-up at provider review bago gumamit ng OTC/supplements.
- Kung gumagamit ng ketogenic o modified Atkins plans, ituro ang praktikal na carbohydrate tracking (madalas napakababa ng total daily carbohydrate limits ayon sa reseta) at i-escalate ang concerns tungkol sa diet tolerability o recurrent breakthrough seizures.
- Ituro ang tuloy-tuloy na nutrition-lab follow-up para sa pangmatagalang antiepileptic therapy (halimbawa vitamin D/calcium at piling B-vitamin status) upang mabawasan ang deficiency at bone-loss risk.
- Ituro ang emergency response steps para sa family/caregivers at kung kailan tatawag ng EMS.
- Palakasin ang trigger reduction, pagsunod sa driving/machinery law, medical-alert identification, at seizure-diary tracking.
- Iugnay ang families sa community support services tulad ng epilepsy organizations.
- Muling suriin ang outcomes nang tuloy-tuloy at i-revise ang care plans kapag partially met o unmet ang goals.
Clinical Judgment Application
Clinical Scenario
Ang naka-confine na pasyente na may kilalang epilepsy ay nagkaroon ng tonic-clonic seizure na tumagal ng 6 minutes na may cyanosis at walang pagbabalik ng consciousness sa pagitan ng episodes.
- Recognize Cues: Prolonged/recurrent seizure activity na may oxygenation risk.
- Analyze Cues: Malamang ang status epilepticus at maaari itong magdulot ng mabilis na neurologic injury.
- Prioritize Hypotheses: Ang airway at oxygenation stabilization kasama ang emergency seizure termination ang agarang prayoridad.
- Generate Solutions: I-activate ang emergency response, protektahan ang airway, ihanda ang IV benzodiazepine administration, at tuloy-tuloy na monitoring.
- Take Action: Ipatupad ang seizure-safety bundle, idokumento ang timing/findings, at ipaalam ang deterioration.
- Evaluate Outcomes: Humihinto ang seizure activity, nagiging matatag ang oxygenation, at muling sinusuri ang recovery trend.
Mga Kaugnay na Konsepto
- mga anticonvulsant - Pangunahing pangmatagalang pharmacologic seizure-prevention framework.
- febrile seizures - Pediatric fever-associated seizure pattern na may age- at duration-based classification.
- neurological diagnostic testing at mga pagsasaalang-alang sa nursing - Konteksto ng kaligtasan at interpretasyon ng EEG/imaging/lab.
- pagkilala sa karaniwang neurological disorders at prayoridad na pangangalaga - Escalation framework para sa seizure emergencies.
- mga prayoridad sa nursing care para sa neuromuscular impairment - Pagkakapatong sa pag-iwas sa airway at aspiration risk.
- prayoridad na pangangalaga sa meningitis at panganib ng ICP - Maaaring magpasimula ng seizure activity ang infectious etiologies.
Sariling Pagsusuri
- Aling bedside actions ang kontraindikado sa panahon ng active generalized seizure?
- Kailan tumutugon ang seizure activity sa status-epilepticus criteria na nangangailangan ng emergency escalation?
- Aling teaching points ang pinakamabisa sa pagbawas ng breakthrough-seizure risk sa home management?